
DEPARTMENT OF HEALTH & HUMAN SERVICES
Centers for Medicare & Medicaid Services
Center for Medicare
7500 Security Boulevard
Baltimore, Maryland 21244-1850
DATE: June 18, 2025
TO: Medicare Advantage Organizations, Prescription Drug Plan Sponsors, and Section 1876 Cost Plans
FROM: Kathryn A. Coleman
Director
SUBJECT: Contract Year 2026 Agent and Broker Compensation Rates, Referral/Finder’s
Fees, Submissions, and Training and Testing Requirements
This memorandum provides Contract Year (CY) 2026 agent and broker compensation rates,
referral/finder’s fee amounts, directions for submitting these rates and amounts into the Health
Plan Management System (HPMS), as well as guidance on for MA plans and Part D sponsors for
developing training and testing that satisfies requirements provided at 42 C.F.R. §§422.2274(c)
and 423.2274(c).
On July 3, 2024, the U.S. District Court for the Northern District of Texas issued orders in
Americans for Beneficiary Choice v. HHS , No. 4:24-cv-00439, and Council for Medicare
Choice v. HHS, No. 4:24-cv-00446, which stay for the duration of the litigation the effective date
of certain provisions of the “Medicare Program; Changes to the Medicare Advantage and the
Medicare Prescription Drug Benefit Program for Contract Year 2024-Remaining Provisions and
Contract Year 2025 Policy and Technical Changes to the Medicare Advantage Program,
Medicare Prescription Drug Benefit Program, Medicare Cost Plan Program, and Programs of
All-Inclusive Care for the Elderly (PACE),”, 89 FR 30448 (herein after referred to as the CY
2025 Final Rule). More specifically, the district court’s orders stayed those parts of the CY 2025
Final Rule that amended 42 C.F.R. § 422.2274 (a), (c), (d), (e) and § 423.2274(a), (c), (d), (e).
Therefore, the regulatory language within § 422.2274(a), (c), (d), (e) and § 423.2274(a), (c), (d),
(e) that was effective prior to the issuance of the CY 2025 Final Rule will be in effect for CY
2026 at least as long as the stay is applicable.
As provided in 42 C.F.R. §§ 422.2274(d)(2) and 423.2274(d)(2), the compensation amount an
organization pays to an independent agent or broker for an initial enrollment must be at or below
the fair market value (FMV). 42 C.F.R. §§ 422.2274(d)(3) and 423.2274(d)(3) limit renewal
compensation to a maximum of 50% of the FMV. 42 C.F.R. §§422.2274(f) and 423.2274(f) limit
the amount an organization may pay for referrals.
2
Each year, CMS publishes updated FMV amounts for initial and renewal compensation as well
as referral fees. The amounts below are calculated based upon the methodology in place prior to
issuance of the CY 2025 Final Rule, as described in 42 CFR §§ 422.2274(a) and 423.2274(a).
The FMV amounts for CY 2026 are as follows:
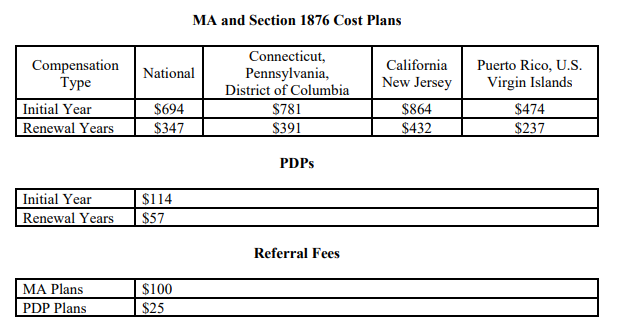
NOTE: CMS rounded the FMV amounts for CY 2026 up to the nearest dollar. The Initial Year
amount is the maximum allowable amount that organizations may pay for enrollments during
compensation cycle-year 1. The renewal amount is the maximum allowable amount that
organizations may pay for enrollments during compensation cycle-years 2 and beyond, for a likeplan type
42 C.F.R. §§ 422.2274(c)(5) and 423.2274(c)(5) require organizations to report to CMS whether
the organization intends to use employed, captive, or independent agents or brokers in the
upcoming plan year along with the specific rates or range of rates the plan will pay independent
agents and brokers. In addition, if an organization pays referral fees, they must disclose the
amount. The regulations state that organizations must provide this data to CMS by the last Friday
in July which would be July 25, 2025, for the 2026 plan year.
CMS has provided instructions for data entry in the HPMS Marketing Module User Guide.
Organizations must submit their agent/broker information in the HPMS Marketing Module
between June 2 and July 25, 2025, 11:59 pm EST. Please note that CMS does not consider the
submission process complete until the organization’s CEO, COO, or CFO has completed the
attestation in HPMS. Organizations that fail to submit and attest to their agent and broker
compensation data by 11:59 pm EST on July 25, 2025, will be out of compliance with CMS
requirements. Furthermore, organizations may not make changes to those submissions after July
25, 2025.
CMS expects organizations to keep full records documenting that they are updating
compensation schedules and paying agents and brokers according to CMS requirements.
Please note that CMS will make the CY 2026 organization-submitted compensation information
available for the public to view at: https://www.cms.gov prior to the annual election period for
CY 2026.
42 C.F.R. §§422.2274(b)(2) and 423.2274(b)(2) require that organizations train and test all
agents and brokers selling Medicare products, including employees, subcontractors, downstream
entities, and/or delegated entities annually on Medicare Parts A, B, C, D, and plan specific
information. Under §§ 422.2274(b)(2) and 423.2274(b)(2), agents and brokers must achieve an
85% or higher score to satisfy the testing requirement.
To assist MA organizations in ensuring the quality of agent and broker training and testing
programs, CMS annually provides minimum training and testing guidelines to organizations.
Organizations should review these guidelines before developing their own agent and broker
training and testing programs to understand the scope of the required training and testing
requirements. CMS encourages organizations, as well as third-party training and testing vendors
used by plans, to include other relevant topics in addition to the minimum elements provided in
CMS’s annual guidelines.
CMS will make the CY 2026 CMS training and testing guidelines available at:
https://www.cms.gov/Medicare/HealthPlans/ManagedCareMarketing/MarketngModelsStandardDocumentsandEducationalMaterial.
Please contact your CMS Account Manager with any questions. For technical assistance with
HPMS submissions, please contact the HPMS Help Desk at: hpms@cms.hhs.gov or 1-800-220-2028.

As a health insurance FMO, we partner with licensed and certified agents to deliver comprehensive onboarding, training, support, and assistance with customer enrollments
Agent Support: +1(972) 432-7151
agent-support@apidesigners.com